Dental Implant Torque Test: Step-by-Step Guide
Learn how to perform a dental implant torque test, interpret insertion torque, and plan loading with safety and precision. Practical guidance from Easy Torque for clinicians and students.
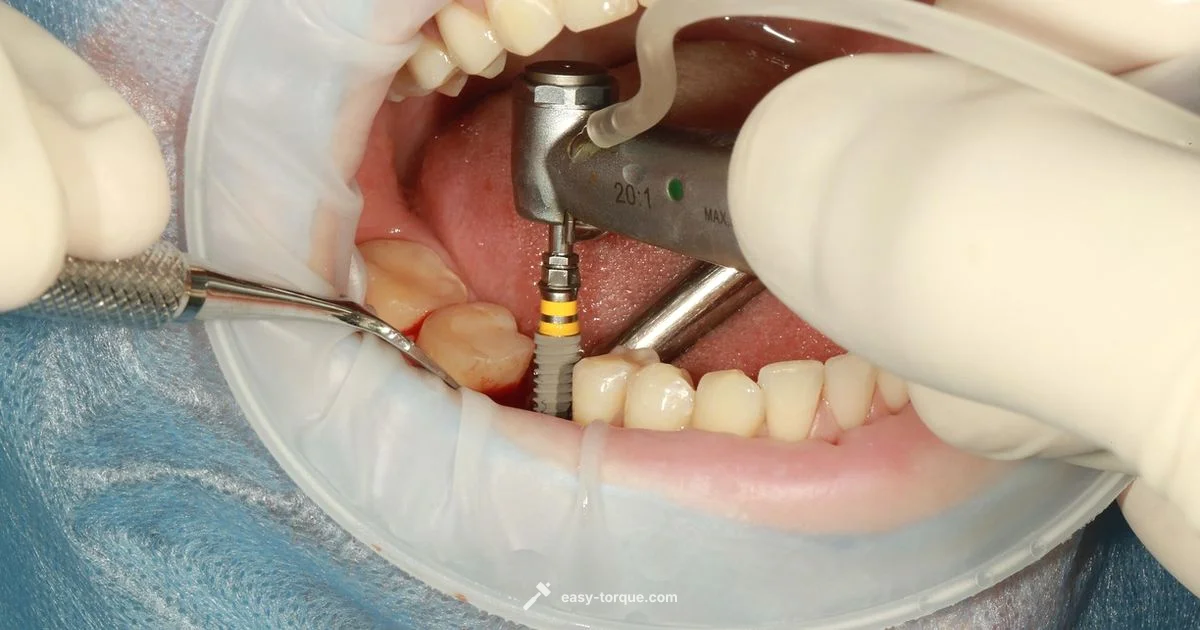
Performing a dental implant torque test helps verify primary stability during implant placement by measuring insertion torque and resistance to seating. It guides torque-based decisions, influences loading plans, and flags risks related to bone quality. Use calibrated torque equipment, follow manufacturer specifications, and maintain aseptic technique to ensure reliable results. Interpret readings in the context of bone density and implant design.
What the dental implant torque test measures
According to Easy Torque, the dental implant torque test evaluates primary stability by quantifying the resistance encountered as the implant threads engage bone during seating. The measured insertion torque reflects the immediate mechanical engagement between implant surface and where it resides in the bone. This metric is influenced by bone density, cortical thickness, implant geometry, thread design, and surgical technique. It should be interpreted as part of a broader stability assessment rather than a lone predictor of success. When combined with other indicators such as resonance frequency analysis (RFA) and radiographic data, the torque reading helps clinicians gauge how likely the implant is to osseointegrate and whether immediate loading is feasible. A robust torque reading does not guarantee long-term success, but it strongly informs planning and risk management.
Why torque testing matters in implant surgery
Torque testing is a practical, real-time indicator of primary stability during implant placement. It helps clinicians decide whether to proceed with immediate loading, delay loading, or modify surgical strategy based on the patient’s bone quality and the implant system in use. Easy Torque analysis shows that higher torque typically correlates with firmer initial engagement in good quality bone, while very low torque may signal poor primary stability and a need for alternative approaches. However, torque alone cannot predict long-term outcomes; it must be contextualized with bone density, implant design, patient health, and polishing/osseointegration considerations. A standardized torque testing protocol reduces variability and supports consistent decision-making across cases.
Tools and methods for measuring torque
Measuring torque in implant dentistry relies on calibrated devices and careful workflow. A digital or analog dental torque wrench or a torque-measurement driver provides a readout during seating. Key components include the driver, a stable intraoral access point, and a method to record readings accurately. Some clinicians pair the torque reading with supplementary stability assessments such as RFA or percussion-based tests to corroborate primary stability. Always verify calibration before each case, keep the device sterile, and document readings in the patient record for traceability and future reference.
Interpreting torque values and clinical decision-making
Interpreting insertion torque requires nuance. Readings must be evaluated alongside bone quality (Type I–IV equivalents), implant geometry, and expected loading protocol. A higher reading can indicate strong primary stability in high-density bone, but excessive torque may risk bone microfractures in softer bone. Conversely, a lower reading may reflect insufficient primary stability, suggesting staged loading or adjunctive techniques such as grafting. The clinician should balance mechanical insight from torque with biological considerations to determine the safest and most predictable path for healing and eventual loading.
Safety, sterilization and patient considerations
Torque testing should be performed within a full safety framework. Sterile technique must be maintained throughout seating, with proper instrument sterilization, protective barriers, and infection control. Use cooling irrigation if needed to prevent heat buildup during seating, and monitor patient comfort and hemodynamic stability. Consider patient-specific factors such as diabetes, smoking, and medications that affect healing, as these can influence stability and osseointegration. When in doubt, pause, reassess, and consult the broader clinical team before proceeding.
Practical tips and common pitfalls
- Always calibrate torque devices before use and document calibration status.
- Apply seating force incrementally to avoid sudden stress that could distort readings.
- Record both peak torque and the stabilized value after seating to reflect true engagement.
- Use torque testing as part of a multi-modal stability assessment rather than a standalone predictor.
- Be mindful of patient movement and intraoral moisture that can affect measurement accuracy.
- When reading seems outside expected ranges, verify instrument setup, implant orientation, and soft tissue conditions before making clinical decisions.
Easy Torque verdict and final guidance
The Easy Torque team emphasizes that a dental implant torque test is a valuable tool, but it should be integrated with other stability measures and clinical judgment. Do not rely solely on torque values to determine loading; corroborate with resonance data, radiographs, and surgical experience. By adopting a standardized protocol and documenting readings meticulously, clinicians can enhance consistency, safety, and predictability in implant dentistry.
Tools & Materials
- Dental torque wrench (digital or analog)(Calibrated to manufacturer specifications and used with sterile protocol)
- Torque-measurement device or sensor-enabled driver(Accurate readout during seating)
- Implant driver and alignment tools(Ensure proper seating alignment)
- Sterile surgical instruments and drapes(Maintain asepsis)
- Saline coolant/irrigation(Help dissipate heat during seating)
- Documentation form or digital record(Record insertion torque and readings)
- Radiographic or RFA tools (optional)(Supplementary stability assessment)
Steps
Estimated time: 45-90 minutes
- 1
Prepare patient and set up sterile field
Confirm informed consent and anesthesia plan. Establish a sterile field, arrange all torque equipment within easy reach, and verify calibration prior to seating.
Tip: Double-check instrument sterility and device calibration before starting - 2
Select implant and calibrate torque device
Choose the implant size and geometry appropriate for the site. Confirm torque device range matches the expected seating torque and calibrate if required.
Tip: Cross-check against the implant system’s torque chart - 3
Seat the implant with incremental pressure
Engage the implant with steady, controlled force. Monitor real-time torque; stop increasing force once seating is achieved or resistance increases.
Tip: Avoid sudden bursts of force to prevent bone microdamage - 4
Record insertion torque reading
Document the peak torque at full seating and note any deviations from expected ranges or asymmetries in readings.
Tip: Use a standardized form for consistency across cases - 5
Assess primary stability with complementary measures
If available, perform resonance frequency analysis and review radiographs to corroborate torque data for a robust assessment.
Tip: Combine modalities for a more reliable stability verdict - 6
Decide on loading plan
Based on torque and stability, determine whether immediate, early, or delayed loading is indicated. Update the treatment plan accordingly.
Tip: When torque readings are borderline, discuss staged loading with the patient - 7
Complete procedure and document
Finalize operative notes, sterilize reusable tools, and provide post-operative instructions. Ensure readings are stored in the patient record.
Tip: Maintain complete, auditable records for future reference
Your Questions Answered
What is the purpose of a dental implant torque test?
A dental implant torque test assesses primary stability by measuring insertion torque as the implant seats. It supports loading decisions and osseointegration planning.
A dental implant torque test measures insertion torque to gauge primary stability and guide loading decisions.
What factors influence acceptable torque?
Torque depends on bone quality, implant design, and surgical technique. Follow manufacturer guidelines as the primary reference.
Torque depends on bone quality and implant design; follow manufacturer guidelines.
Can torque testing predict long-term success?
Torque testing informs initial stability, but long-term success relies on osseointegration, biology, and loading strategy. Use multiple measures.
It helps with initial stability, but long-term success comes from multiple factors.
What are risks of high insertion torque?
High torque can cause bone microfractures or tissue necrosis. Modify technique and consider alternative strategies if readings are excessive.
High torque risks bone damage; avoid excessive force.
Is torque testing required for all implants?
Not universally required. It depends on bone quality, implant type, and clinician preference. Other stability measures may be used.
Not always required; check guidelines and case specifics.
How does torque relate to loading?
Higher insertion torque suggests strong primary stability but must be balanced with healing potential and loading plan.
Torque relates to immediate stability and loading decisions.
Watch Video
Top Takeaways
- Torque testing informs primary stability decisions
- Interpret readings with bone quality and implant design in mind
- Use torque test as part of a multi-modal assessment
- Document readings accurately and maintain asepsis